Durga G, Rajkumar Jini, Nair Amal S, Nair Anjana S
Department of Orthodontics & Dentofacial Orthopaedics, Sree Mookambika Institute of Dental Sciences, Kulasekharam
Running title – Acrylic splint Herbst
Received: 15-06-2023
Revised: 19-06-2023
Accepted: 25-06-2023
Address for correspondence: Dr. Amal S Nair, Sree Shobha, H.S. Road, 2nd house, Kazhakuttom P.O, TVM-695582
Email: amalsnair@gmail.com
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-Noncommercial ShareAlike 4.0 license, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms
How to cite this article: Durga G, Rajkumar J, Nair Amal S, Nair Anjana S. Improving Occlusion and Function with Acrylic Splint Herbst: A Case Report. J Oral Biomed Sci 2023; 2(2): 92-98
Abstract
The Herbst appliance, introduced by Emil Herbst, reintroduced by Pancherz, a widely recognized orthodontic treatment modality, has shown remarkable success in correcting Class II malocclusions and improving mandibular growth in growing patients. This case report presents the application and outcomes of an acrylic splint Herbst appliance in a 16-year-old male patient with a skeletal Class II malocclusion and mandibular retrusion.
The patient presented with a convex facial profile, increased overjet, and a reduced mandibular plane angle. The treatment plan involved the use of an acrylic splint Herbst appliance introduced by J A McNamara, designed to facilitate the advancement of the mandible and promote favorable growth. The treatment duration of acrylic splint herbst appliance (Phase I) spanned 7 months, with monthly follow-up appointments to monitor progress. Following treatment, significant improvements were observed in both the patient’s facial profile and occlusal relationship. The overjet was reduced, and the mandible showed significant advancement. Cephalometric analysis revealed a positive change in the sagittal and vertical dimensions. This was followed by fixed orthodontic appliance therapy (Phase II)
The case report demonstrates the successful application of the acrylic splint Herbst appliance as an effective and well-tolerated treatment option for correcting Class II malocclusions and stimulating mandibular growth in growing patients.
Keywords: Herbst appliance, malocclusion, mandibular growth
INTRODUCTION:
Emil Herbst, a German professor, made the introduction of the Herbst appliance at the International Dental Congress in Berlin in 1905.The Herbst appliance- a non compliance class II corrector works twenty four hours a day and requires no patient co-operation, and only takes about six to eight months for a class II correction. The Herbst appliance is extensively accepted in modern orthodontics for Class II therapy when Hans Pancherz reintroduced it in 1979. Comparing the appliance to removable bite-jumping devices (functional appliances), such as the activator, bionator, and Frankel appliance, there are various advantages.1There is a significant need for a therapy that has a treatment time that is as predictable as possible and is as compliance-independent as possible. After the pubertal development peak, fixed devices for Class II correction offer an alternative for treating this form of dysgnathia, and are also suitable in adulthood to avoid a surgical treatment for Class II correction. The fixed Class II mechanics were further developed and varied due to their efficacy for the dentist, integration into daily practice, and quick and good effectiveness. 2,3
According to research so far, the Herbst appliance prevents maxillary anteroposterior growth and enhances mandibular length, and resulting in a appropriate facial height. According to early findings, mandibular growth stimulation was predominantly responsible for Class II correction. Due to issues with mandibular incisor proclination and band breaking according to the original herbst appliance design, there has been further modifications by various authors. The usage of stainless steel crowns on the maxillary first molars and an occlusal coverage bonded splint on the mandible have both been modified. This bonding technique decreased mandibular incisor proclination.4-6
More recently acrylic splints have been used as the bite-jumping mechanisms on both the maxillary and mandibular dental arches. To avoid decalcifications, it is advised to avoid bonding of splints of maxillary and mandibular arches or atleast avoid bonding of splints of mandibular arches.7,8
Case Report:
A 16 years old male reported to the Post graduate Clinic of Department of Orthodontics and Dentofacial Orthopaedics, Sree Mookambika Institute of Dental Sciences with the chief complaint of forwardly placed teeth in upper front tooth region for past 6 years.
His parents are alive and healthy. He has one elder sister. General health of the family was reported to be normal. No relevant history for similar dental condition in the family. The attitude of the patient towards the treatment was highly positive. The delivery was full term and C section and with no complication during and after delivery. There was no history of Rh incompatibility or any other congenital anomaly.
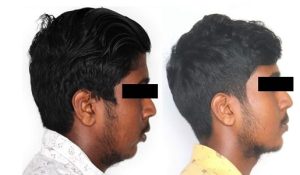
On General Examination, the patient was moderately built with erect and upright posture. In profile view, face was convex with posterior divergence. The inclination of mandibular plane to Frankfort horizontal plane was high and chin appeared average. When examined together lips were Potentially incompetent with an interlabial gap of 4 mm. (Fig 1)
On Intraoral Examination, The oral and buccal mucosa appeared to be normal with no high frenal attachments. Colour and texture of gingiva appeared to be with blackish pigmentation with no periodontal pockets. Attached gingiva was of adequate width. Intraoral examination showed permanent dentition with Angles Class II Div 1 malocclusion with an overjet of 7 mm. Functional examination revealed normal function, mastication & speech. Maximum interincisal opening was 46 mm with free way space of 2 mm.(Fig 2)
On Radiographic examination, cephalogram revealed well defined outlines of the hard & soft tissues of the skull. Concavities at the lower borders of C2, C3, and C4 are now present. The bodies of both C3 and C4 are vertically than horizontally in shape indicating maturation stage. Further examination of the cephalogram revealed normally positioned maxillary apical base in relation to the anterior cranial base as indicated by the SNA value of 84o and posterior positioning of the mandibular apical base in relation to the anterior apical base as indicated by SNB value of 76o, ANB of 8o was suggestive of Class II maxillomandibular skeletal relation. Soft tissue analysis showed average nasolabial angle with value 104 degree. FMA showed a value of 36 indicating vertical growth pattern. ( Fig 3)
Diagnosis:
Based on clincal and radiographic examination, the final diagnosis was concluded to be a circumpubertal male with Angle’s Class II Division 1 malocclusion on a class II skeletal base due to retrognathic mandible with vertical growth pattern along with crowding in upper and lower arch, deep bite and scissor bite in relation to 25,35 with convex profile and potentially incompetent lips.
Treatment objectives:
The main Objective was to correct the Skeletal Class II relation due to retrognathic mandible and to obtain a pleasing profile. Dentally, the objective was to obtain a class I canine and class I molar relationship in right and left side and to correct proclined upper and lower incisors, Scissor bite in relation to 25,35 and to correct midline diastema. The objective was also to achieve a pleasing soft tissue profile. Treatment was planned in two phases- Phase I- Acrylic splint herbst therapy ( Fig 4) followed by Phase II- Fixed Orthodontic Appliance Therapy.
Progress:
At the end of phase I pleasing profile and class I molar relation was achieved.(Fig 5) On Radiographic examination at the end of phase I therapy, Lateral cephalogram revealed normally positioned maxillary apical base in relation to the anterior cranial base as indicated by the SNA value of 83o and posterior positioning of the mandibular apical base in relation to the anterior apical base as indicated by SNB value of 80o, ANB of 3o was suggestive of Class II maxillomandibular skeletal relation. Soft tissue analysis showed average nasolabial angle with value 90 degree. FMA showed a value of 34 indicating vertical growth pattern.
As Phase II therapy, Fixed orthodontic appliance treatment was started as a non extraction treatment with 0.022 MBT Pre adjusted edgewise prescription was started for dental correction of proclination and crowding ( Fig 6). After and aligning, levelling and space closure, another radiographic examination (Fig 7) was carried out before debonding. The Class I molar was achieved at the end of Phase I therapy and was maintained throughout the Fixed orthodontic appliance therapy ( Phase II)
Discussion:
Herbst therapy with acrylic splint is a successful method for treating Class II malocclusion. The majority of the treatment’s effects are skeletal and result from change to the mandibular dimensions (total mandibular length and ramus height) and mandibular sagittal position. The mandibular dental arch’s mesial movement is crucial for molar relationship and overjet correction. 9 Slight proclination and forward bodily movement of the mandibular incisors were noted with no significant change occurring in the maxillary incisors. Significant distal bodily movement and tipping of the maxillary first molars occurred, while the mandibular first molars demonstrated significant mesial bodily movement with minimal tipping. According to J A McNamara, a forward advancement of the mandible will result in the lower incisors being displaced downward and forward along the lingual aspect of the upper incisors. This movement will increase the vertical dimension of the patient and may result in a posterior open bite existing at the time of appliance removal. 10-14 The same was observed in this patient after the removal of the appliance. After the treatment with Acrylic splint herbst appliance, there is a significant improvement in soft tissue as well as skeletal relation when examined radiographically.15-17 The patient achieved a good soft tissue profile (Fig: 8) and dental corrections with Fixed orthodontic appliance therapy was achieved.
CONCLUSION:
The Herbst appliance aids in the correction of Class II skeletal problems by eliminating the need for patient cooperation, provide the ability to stimulate the overall amount of mandibular growth by remodeling of glenoid fossa and mandibular condyle 18 , and direct this growth in the appropriate direction. According to studies by Valant et al(1989), The acrylic splint herbst gives a lesser mandibular anterior proclination and no significant change in maxillary anteriors.
Conflict of interest: None
Source of support: Nil
REFERENCES:
- Pancherz H. The Herbst appliance—Its biologic effects and clinical use. Am J Orthod. 1979;76:423-442.
- Pancherz H. Treatment of Class II malocclusions by bite jumping with the Herbst appliance: a cephalometric investigation. AM J ORTHOD 1979;76:423-42.
- Pancherz H. The mechanism of Class II correction in Herbst appliance treatment: a cephalometric investigation. AM J ORTHOD 1982;82:104-13.
- Langford NM. The Herbst appliance. J Clin Orthod 1981;15:558-61.
- Howe RP. The bonded Herbst appliance. J Clin Orthod 1982;16:663-7.
- Howe RP. Updating the bonded Herbst appliance. J Clin Orthod 1983;17:12;1-4.
- Fabrication of the acrylic splint Herbst appliance, J A McNamara Am. J. Orthod. Dento. Orthop.1988 4:10-8.
- Clinical management of the acrylic splint Herbst appliance, J A McNamara Am J Orthod Dentofacial Orthop 1988 ;94:142-9
- Treatment and posttreatment effects of acrylic splint Herbst appliance therapy, Lorenzo Franchi, Am J Orthod Dentofacial Orthop 1999;115:429-38
- Treatment effects of the Herbst Appliance John Valant, Am J Orthod Dentofac Orthop 1989;95:138-47.
- Janson G, Branco NC, Freitas MR. Mandibular skeletal changes after Herbst appliance treatment—a systematic review. Eur J Orthod. 2005;27:247-252.
- Ruf S, Pancherz H, Kohlhas P. “Effective” Herbst treatment: 10-year dentofacial changes in relation to treatment duration. Am J Orthod Dentofacial Orthop. 1998;114:689-698.
- McNamara Jr JA, Baccetti T, Franchi L, Herberger TA. A cephalometric and tomographic evaluation of two protocols for treating Class II Division 1 malocclusions. Am J Orthod Dentofacial Orthop. 2003;123:670-678.
- Cunha AC, Santos-Pinto A. Dentoskeletal effects of the Herbst appliance—a cephalometric evaluation. Eur J Orthod. 2005;27:176-182.
- Ken Hansen, Hans Pancherz, Long-term effects of Herbst treatment in relation to normal growth development: a cephalometric study, European Journal of Orthodontics, Volume 14, Issue 4, August 1992, Pages 285–295.
- Yang X, Zhu Y, Long H, Zhou Y, Jian F, Ye N, Gao M, Lai W. The effectiveness of the Herbst appliance for patients with Class II malocclusion: a meta-analysis. Eur J Orthod. 2016 Jun;38(3):324-33.
- Ruf S, Pancherz H. The mechanism of Class II correction in Herbst appliance treatment. A cephalometric investigation. Am J Orthod Dentofacial Orthop. 1982;104-113.
- Ruf S, Pancherz H. Temporomandibular joint growth adaptation in Herbst treatment: a prospective magnetic resonance imaging and cephalometric roentgenographic study. Eur J Orthod. 1998.
FIG 1: PRETREATMENT PHOTOS – EXTRAORAL
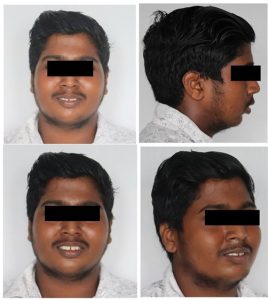
FIG 2: PRETREATMENT PHOTOS – INTRAORAL

FIG 3 LATERAL CEPHALOGRAM – PRETREATMENT
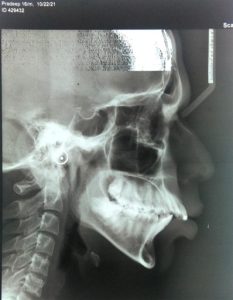
FIG 4: ACRYLIC SPLINT HERBST APPLIANCE
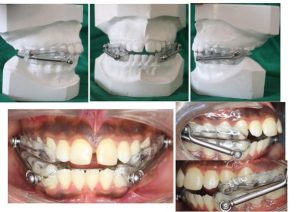
FIG 5: END OF PHASE 1- INTRAORAL PHOTOGRAPHS
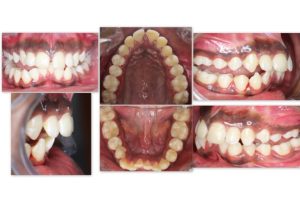
FIG 6: PHASE II – BONDING
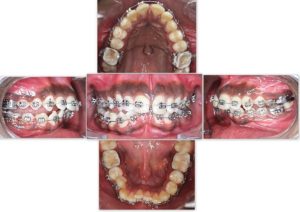
FIG 7: PREDEBOND RADIOGRAPH:
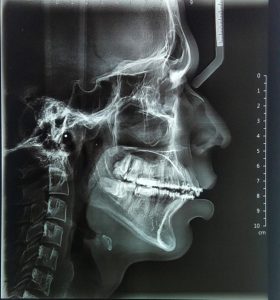
FIG 8: PRETREATMENT VS POSTTREATMENT PROFILE: